A Brief Guide to Egg Donation: What to Know (for Donors and Recipients)
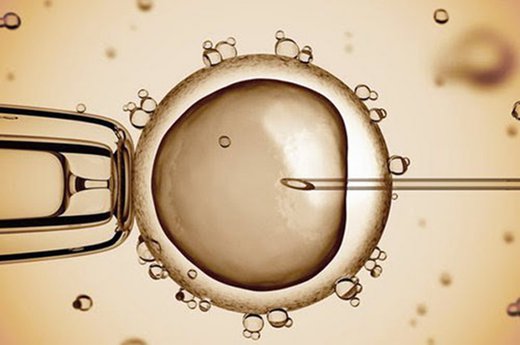
Egg donation is defined as the process where a woman’s ovaries are stimulated to produce multiple mature eggs, which are then harvested and donated, usually for the purpose of assisted or third-party reproduction. Eggs may be frozen for later use or fertilized in vitro (in a laboratory).
Though initially plagued by controversy, the science behind in vitro fertilization (IVF) and oocyte (egg) and embryo donation has completely changed the future of reproductive medicine and now provides a new platform for advancements in women’s health.
Today, it’s about women (the donors) helping people (of all orientations and relationship statuses) to overcome infertility challenges with the aid of technology.
In the decades since the first IVF pregnancy and subsequent birth, egg and embryo donation have become as commonplace as major organ donation. Women may choose to become an egg donor for any number of reasons, and the donated eggs can then be fertilized and implanted immediately or frozen for later use.
Research tells us that egg quality and quantity are closely related to a woman’s age. Women are born with all the eggs they will ever have and their quantity decreases over time. A woman’s fertility generally begins to decline in her mid-thirties and continues to accelerate. Though the woman may still be fertile, the quantity of available eggs decreases and the quality of the available eggs drops. Chromosomal abnormalities also increase markedly with age and women who wish to have children later in life may require the exploration of other options for becoming pregnant. At this stage, some women may explore the possibility of donor egg IVF, either by seeking out a fresh egg donor through a local program or utilizing a frozen egg bank.
A Brief History of ART & Egg Donation
ART has advanced in stages, with the earliest reported attempt dating back to 1790 when a Scottish doctor inseminated a woman with her husband’s sperm. Nearly one hundred years later, in 1884, a woman was inseminated with donor sperm.
In 1944, pioneering physicians John Rock and Miriam Menkin reported the first in vitro fertilization of a human egg, though no pregnancy resulted.
In 1954, we saw the first successful pregnancy using frozen sperm and in 1978, the first baby conceived through IVF was born.
The first pregnancy from a donated egg was reported in Australia in 1983, while the first successful birth occurred one year later in California, the result of a procedure that transplanted an already-fertilized egg from one woman to another. Performed at UCLA Medical Center, the birth heralded a new era for single women, infertile couples and same-sex couples who wished to start a family. Prior to this breakthrough, the only option available to these parental hopefuls was adoption or surrogacy. For women who were unable to become pregnant or who were at risk of passing on various genetic disorders, this new approach opened the doors to exciting new possibilities.
More Recently
Since that first birth from a donated egg, there have been more than 50,000 live births from donated eggs. As the practice became more widespread, much legislation has been debated and passed into law. The American Society for Reproductive Medicine (ASRM) established guidelines for the procedures involved, as did the Food and Drug Administration. As a result, many women travel to the US from foreign countries that do not allow compensation of an egg donor’s time and inconvenience. For many donors, the practice is purely altruistic, but it can also provide some attractive financial benefits.
Indications for Donor Eggs
The typical recipient of donor eggs can be categorized into several subsets:
Women who have previously had multiple unsuccessful in-vitro treatments. Poor egg quality and genetic abnormalities may be a contributing factor in the failure to conceive by this method.
Secondary infertility, defined as when one child is conceived naturally but a second attempt is unsuccessful. There can be many causes of secondary infertility including age, structural complications such as endometriosis, sperm quality and quantity, weight gain and smoking.
Premature ovarian failure (menopause before the age of forty).
Women affected by reproductive abnormalities that would cause them to not produce viable eggs.
Male same sex couples.
Other unexplained infertility issues.
Preparation for Egg Recipients
A full medical evaluation is necessary for all women who hope to conceive using donor eggs.
A complete physical exam should conclude that their health will not be significantly jeopardized by a pregnancy. A full range of testing may include a cervical culture, a hysteroscopy and a hysterosalpingogram or saline sonogram to assess uterine health. Semen testing should also be performed on the male counterpart to rule out any contributing factors. Some clinics will order a course of hormone replacement prior to the actual embryo transfer: called a ‘prep’, ‘mock’ or ‘dummy’ cycle, it is used to ensure that the hormonal treatment will achieve the desired blood levels and endometrial effects. Some doctors will elect to perform an endometrial biopsy during this cycle to measure the thickness of the endometrial stripe. Preparations should always include a thorough explanation and discussion of the procedural aspects as well as an exploration of the psychological and social impacts of third-party reproduction.
Not all women need an egg donor and if she is still young enough personal egg freezing may still be indicated. Of the women who are physiologically able to conceive, some prefer to take control of the event and make it happen at a time of their own choosing. Depending on the individual situation, many women are choosing to freeze their eggs while they are in their twenties or thirties, the age at which eggs are considered to be the highest quality and most viable. Eggs are retrieved in the same surgical procedure as egg donation and similarly are frozen for use at a later date. For those women who froze their eggs in their younger years and are unsuccessful, donor eggs could still become part of their future journey.
Egg Donation Risks
Of course, as with all medical procedures, minor risks should be considered when electing to pursue donor egg IVF. Whether you are choosing to use fresh or frozen donor eggs, there is about a 50% chance that any given cycle will result in a pregnancy. There is also a possibility of a pregnancy with multiple babies, which carries the added potential for premature delivery, low birth weight, miscarriage or developmental difficulties in the child, and raised blood pressure or gestational diabetes for the mother. Because of this, most physicians will not implant more than two embryos at one time.
What is the Profile of an Egg Donor?
Each egg donor has a different reason for choosing to be a donor. For the vast majority of donors, it is an altruistic endeavor, while for a few others, it is the promise of a financial payment. Why does a donor donate? Typically, she is drawn to make a donation because she knows someone who has struggled to have a baby or perhaps she has chosen to abort a baby and is seeking some level of atonement. Many donors are mothers themselves and can’t imagine life without their children. Giving the gift of life is a powerful motivator and helping others in need is self-fulfilling.
Donors who enter the process for only financial gain are quickly dismayed at the time commitment and physical requirements to be a donor. These women will often drop out during the process as the financial gain does not always fully compensate for the time and inconvenience. For those that continue on, typically the motivating factor is the desire to further their education and the compensation makes additional schooling possible.
Not just anyone can be an egg donor. There are several requirements that screen out donors to include medical physical examinations, drug screening, multi-generational medical history screening, genetic screening and an in-depth psychological evaluation and test is performed to ensure that only appropriate candidates advance to the donation phase. In addition, each potential donor must submit an application that provides information on work history, education, and personal background. This information is provided to the recipient in order to give them the opportunity to make the best possible choice for their family. It should be noted that the donor is relied upon to provide truthful information. Because of today’s health protection laws and privacy laws, DEB USA is unable to validate the truthfulness of the donor’s responses.
To Tell or Not to Tell
The decision to use a donor’s egg to achieve a family is an important one and typically private.

Current research suggests that children told about their genetic origins while young fair better going into adulthood. Nonetheless, no one can force the intended parent to tell their child and the implications of this decision should be weighed, particularly as it relates to the medical history of the child and future medical treatment decisions which could be contradicted or enhanced if the donor’s history were known. Making the decision to not tell should be researched and decided with caution knowing the future risks.
Some intended parents not only intend to tell their children but also desire open relationships with the donor. Open release programs in which the donor has agreed to a mediated meeting at the age of majority are now available. If this is important to the intended parent, then a donor who has opted into this program is a better fit over a donor who has not elected to participate.
The Donor Sibling Registry is also a great resource for donors and intended parents who wish to meet. Registry is a nominal fee and each party can individually place their information online with the hope of a future match. Many half siblings have been found through the registry.
Single Women and LGBT Communities Benefit from Egg Donation
While there are many couples that can benefit greatly from donated eggs, it also serves as a family building option for women who wish to be a single parent and those in the LGBT community.

The ability to build a family with a biological connection, as opposed to adoption, is an exciting option for both communities. Increasingly women over the age of 40 who may not have found Mr. Right are “having it all” on their own terms. Using a combination of donor egg and donor sperm, these women are conceiving and birthing children at historical rates. In addition, egg donation has been revolutionary in the same sex community and men having babies through the use of a gestational carrier is on the rise.
Meanwhile, lesbian couples are using donor eggs; sharing the pregnancy with one being the donor and the other the carrier. With the added family security that comes with the legalization of same-sex marriage, many couples are becoming more interested in building their family unit within the institution of marriage. For LGBT couples, egg donation is a happy and exciting process, as opposed to heterosexual couples, where it often comes after years of inability to conceive. But the common ground between them all is the desire to have a healthy child.
What Egg Donors and Recipients Should Look Forward To
The process of egg donation is two-fold: for egg donors, it is a chance to help others achieve their most cherished dreams. For the egg recipients, it is a chance to conceive, start a family and complete a picture of happiness. Essentially, it is making the impossible possible.
There are several questions that concern many couples considering donated eggs that include whether the recipient will truly feel that the child is theirs, how can they approach the inevitable discussion about how the conception took place and several others. These are great questions to discuss with a reproductive psychologist. Many women and men have conceived via donor egg IVF and the good news is there is a community of supporters at Parent’s Via Egg Donation (PVED) who are willing to help intended parents navigate these tricky questions. As for will the baby feel like yours? Click our video to find out.
You might say that the donor is the genetic contributor, but the person who carried the child is truly the biological mother.
While there is a delicate balance to be struck, one fact remains: this child was brought into the world with great thought, love and intent from many sources.Categories
Latest Posts
- Pride, Parenthood and Possibility: A Guide for Gay Dads Using Frozen Donor Egg
- Victoria’s Story: Choosing Donor Egg and Beyond
- Heartbreak, jealousy, and then one ‘golden egg’. How actress Camille Guaty finally became a mom with donor egg
- Empowering Your Family Dreams: Accessing Fertility Coverage Made Simple
- Donor Egg Bank USA’s Partner Summit 2024
- Planning, Painting and Picking: A Donor Egg Bank USA Employee’s Journey to Motherhood
- Real Stories: A Path to Parenthood Through Donor Eggs
- Mental Health and Infertility 101: What You Should Know
- Mark Yourself as a Resource During National Infertility Week®
- 5 Reasons It’s Not Your Fault You’re Not Pregnant
Comments
Nice blog.
Submitted by Physician's Surrogacy 6 years, 8 months ago
Share Your Thoughts